Trump/GOP Plans For Obamacare, Medicare, & Medicaid Have Far-Reaching Pharma Effects

By Paula Wade, Decision Resources Group
As U.S. President-elect Donald Trump and emboldened Republican (GOP) Congressional leaders plan their first-100-days agenda of repealing and replacing Obamacare, they’re acting a bit like a dog that finally caught the mail truck.
With the White House and solid GOP majorities in Congress, House Speaker Paul Ryan announced that he is ready to push through the GOP’s long-touted health policy trifecta: to end Obamacare and completely redefine Medicare and Medicaid.
GOP officials campaigned to bring Obamacare repeal on “day one,” never acknowledging the complexities of the task or designing its long-promised replacement. Ryan’s plans for Medicare and Medicaid are more concrete: Instead of guaranteeing comprehensive medical coverage to those who qualify, Ryan’s plans would convert Medicare into a premium assistance voucher program and Medicaid into a state block grant with few strings attached.
These three changes would substantially reduce or eliminate access to healthcare for millions of Americans and create a cascade of potential consequences to hospitals, insurers, physicians, pharmaceutical companies, and others in the healthcare sector. Taken together, the potential effects and implications of these changes are not even fully known to these industry stakeholders, much less to American voters.
So despite Trump’s and Ryan’s vows to move quickly on repeal of the entire ACA, insurers have convinced Senate members to press for a phased-in repeal/replacement — possibly over the next two to three years — in order to avoid catastrophic disruption in the health insurance market. GOP hard-liners, led by Ryan and Trump’s U.S. Department of Health and Human Services (HHS) nominee Tom Price, will likely push some Obamacare repeal measures through the budget reconciliation process, which needs only 50 Senate votes to be approved, to declare victory.
The GOP’s policy plans do not share Obamacare’s goal of near-universal comprehensive health coverage. Their goal — as expressed in Ryan’s “A Better Way” proposal and Price’s detailed bill on replacing the ACA — is to promote market-based private insurance coverage, less government regulation, budgetary savings, and reduction of government entitlements. That will ultimately result in more people without insurance coverage, and less robust coverage for many who have comprehensive benefits now. What’s unknowable is the extent, and the timetable, of these major changes.
The ideology-driven rush to undo decades of healthcare policy — and the uncertainty this will create — presents real hazards for every segment of the U.S. healthcare system, including the pharmaceutical industry.
The most immediate and obvious hazard for pharma will be a paralyzing uncertainty over Americans’ access to and reimbursement of prescription drugs. That uncertainty endangers pharma’s ability to plan, to estimate the potential market for drugs in development, and to make pricing decisions that depend on projections of covered lives for years after a new drug’s launch.
To understand the potential effect of these changes on the pharma industry, it’s helpful to understand how each piece in the GOP health reform trifecta stands to change the healthcare landscape for pharma.
U.S. Population by Health Coverage Type, 2016
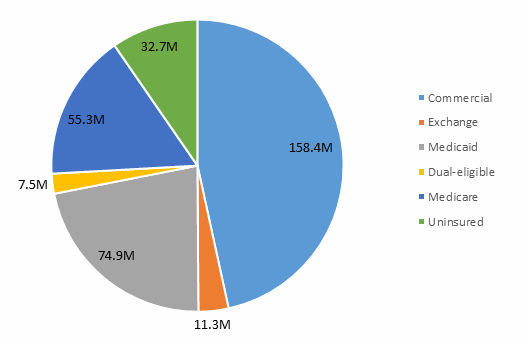
Source: DRG Managed Market Surveyor, January 2016
Obamacare: Repeal Sounds Easy, Except Its Replacement Doesn’t Exist
Eager to fulfill his campaign promise to repeal Obamacare, Trump is expected to use his executive powers to nullify or undermine sections of the ACA that the administration has the power to change. GOP leaders in Congress are expected to repeal parts of the law via budget reconciliation — a method that avoids the prospect of a Senate filibuster — with transition periods phasing out the law’s many provisions.
Congress is likely to allow coverage to continue through the end of 2017 for the ~20 million Medicaid expansion enrollees and subsidy-supported exchange members already enrolled as of January 2017. But beyond that, it is impossible to know how quickly these individuals will lose their Medicaid eligibility or ACA subsidies.
Potential budget-reconciliation targets include:
- Eliminating the requirement that individuals purchase health insurance and/or eliminating the penalties for remaining uninsured
- Eliminating enhanced Medicaid matching funds for the Medicaid expansion population (an action that shifts the cost to state budgets, exerting pressure for states to abandon the expansion)
- Eliminating or reducing subsidy funding for 2018 exchange enrollees, making the plans unaffordable for millions of current policyholders
- Expanding risk mitigation for exchange insurers long enough to keep the market steady during a two-year phase-out of the ACA
“Replacement” of the ACA law will be a long legislative slog, requiring the support of at least eight Senate Democrats for filibuster-proof passage. Republican replacement ideas include encouraging greater use of medical savings accounts, instituting publicly supported high-risk pools, relaxing minimum benefit requirements for insurance policies, and allowing purchase of plans across state lines.
While Trump and Congressional Republicans express support for the popular ACA provision that assures coverage for those with pre-existing conditions, they are likely to allow insurers to again price their premiums based on age, gender, medical status, and claims history. In other words, individuals with medical conditions might apply for coverage but would be unlikely to afford it.
Trump has pledged to eliminate government regulation and could choose to ignore discriminatory health plan formularies that exclude high-cost medications or drugs used by those with high-cost illnesses.
Medicaid: Block Grants Would Let States Reduce Benefit Levels, Eligible Populations
For years, Ryan and other Republicans have promoted changing Medicaid — the source of comprehensive healthcare for more than 75 million Americans — into a block-grant program controlled by states, ending the Medicaid entitlement. For the medical industry, the change would result in state Medicaid programs that offer vastly different benefits state-to-state, and that can be altered by state legislators each year depending on fluctuating state budgetary and political conditions.
Since its inception, Medicaid has guaranteed “all medically necessary covered services” to those who qualify for the state-federal program. Federal law requires that some categories of people be covered — needy families qualifying for assistance, children in foster care, the aged, blind and disabled and other categories — but allows states to cover other groups if they wish. But state-led expansions have been held in check by cost.
The ACA expanded Medicaid by extending coverage to those under 138 percent of the federal poverty level, with the federal government paying 100 percent of the cost for that expansion population. When the Supreme Court held that states could exempt themselves from the ACA expansion, many Republican-led states did so. Today, 31 states and the District of Columbia have expanded coverage.
State officials have at times chafed at the fact that Medicaid rules require coverage of expensive care, such as organ transplants and expensive medications (e.g., Sovaldi). Without the federal mandate to provide “all medically necessary” services, some states will rush to save money by setting a lower standard of care — such as a finite list of covered services, benefit caps, exclusions of high-cost treatments, or coinsurance for high-cost medications (out of reach for most Medicaid beneficiaries).
Under the Medicaid reform plan proposed by the House GOP, states could choose to receive a static block grant amount or a capped per-enrollee amount from the federal government, but could have significant flexibility to determine who is eligible, impose work requirements, charge monthly premium payments, or require drug testing.
Even without federal legislation, Trump could loosen federal Medicaid waiver requirements to allow states to charge premiums (as Indiana already does), impose work requirements, or deny Medicaid re-enrollment until any premium arrears are paid. For Medicaid enrollees, such changes often function as hurdles that trigger dis-enrollment, loss of coverage and interruptions in needed care.
Medicaid accounts for roughly 9 percent of prescription drug spending in the U.S., with high spending in antivirals, antiasthmatics and bronchodialtors, ADHD drugs, antispychotics, and antidiabetics (Kaiser Family Foundation). Under federal law, pharmaceutical companies must provide their lowest prices to the Medicaid system.
Medicare: Here’s Your Voucher — Let’s Go To The Computer And Look For Some Insurance!
The ultimate irony of House Speaker Ryan’s voucher plan for Medicare is that it works a great deal like Obamacare’s insurance subsidy program: Beneficiaries would receive a voucher worth a certain amount and would use that money to help pay for insurance from a private insurer. (Ryan avoids the use of the word “voucher” to describe what his proposal does, but the word fits.)
Ryan is pitching his Medicare voucher plan as part of the ACA repeal, arguing that “because of Obamacare, Medicare is going broke.” (Actually, the opposite is true: ACA changes extended the Medicare trust fund’s solvency by more than a decade.)
Medicare was created in answer to the actuarial reality that it’s impossible to design an affordable health insurance risk pool for the elderly because of their significant medical needs. Voucherized private insurance for Medicare-eligibles is vastly different from today’s privatized Medicare Advantage program, in which insurers are paid risk-adjusted per-member payments by Medicare, and then can receive additional risk-based payments if they can document that their members had higher medical risk than anticipated.
The implication is that Medicaid voucher plans would function similarly to individual commercial coverage, with the more affordable plans featuring high deductibles, cost-sharing, restrictive networks, and lower benefit levels. The Medicare voucher proposal is the most politically risky of Ryan’s proposals and would likely be designed to affect only those becoming Medicare-eligible beyond a future date — a provision that exempts those currently receiving benefits.
The potential effect on medical and pharmaceutical access for seniors is obviously a significant unknown, but because Medicare accounts for nearly 30 percent of all pharmaceutical spending, the potential reduction in access and reimbursement cannot be ignored.
Pharmaceutical companies are already considering their Trump-era lobbying and marketing strategies, increasing payment-assistance programs in expectation of lower rates of insurance, as one example. But pharma’s longer-term pipeline challenge will lie in making a range of assumptions about future covered lives, access, and reimbursement under various policy scenarios going forward.
Hang on tight.
 About The Author:
About The Author:
Paula Wade is principal analyst for Decision Resources Group, analyzing U.S. national healthcare trends and the major national payers. She is the author of DRG’s MCO Analyzer report series and of several Physician/Payer Dynamics reports. She can be found on Twitter at @PaulaWadeDRG.
Image credit: Donald Trump at Aston, PA September 13th (Sean Sullivan and Robert Costa, 2016, CC BY 2.0)
